
Find out more about the potential risks and side effects of omeprazole and thrombocytopenia. Learn how to protect your health and make informed choices about your medication.
Key Facts on Thrombocytopenia
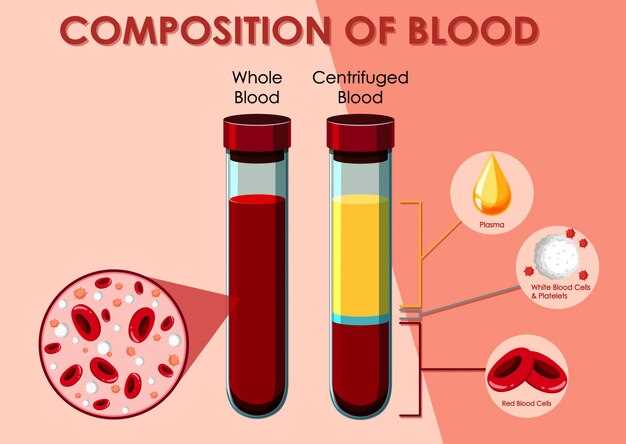
Thrombocytopenia is a medical condition characterized by a low platelet count in the blood.
Platelets are crucial for blood clotting and preventing excessive bleeding.
Thrombocytopenia can result in increased risk of bleeding, bruising, and other complications.
Common causes of thrombocytopenia include autoimmune disorders, infections, medications, and underlying health conditions.
Diagnosis of thrombocytopenia is usually confirmed through a blood test to measure platelet levels.
Treatment of thrombocytopenia depends on the underlying cause and may involve medications, blood transfusions, or other therapies.
Key Facts on Thrombocytopenia
Thrombocytopenia, a condition characterized by low platelet count, can be caused by various factors including medications like omeprazole.
Platelets are essential for blood clotting, and a low platelet count can lead to increased risk of bleeding and bruising.
Thrombocytopenia can be asymptomatic or present with symptoms like easy bruising, nose bleeds, and prolonged bleeding from minor cuts.
It is important to monitor platelet levels and seek medical attention if symptoms of thrombocytopenia are present.
Understanding the causes and risk factors of thrombocytopenia, including the role of medications like omeprazole, can help in timely diagnosis and management of the condition.
Role of Omeprazole in Thrombocytopenia
Omeprazole is a proton pump inhibitor commonly used to treat conditions such as acid reflux and ulcers. While omeprazole is generally considered safe and effective, there have been reports linking its use to thrombocytopenia, a condition characterized by low platelet levels in the blood.
Omeprazole-induced thrombocytopenia is thought to occur due to a hypersensitivity reaction in some individuals. This reaction can lead to the destruction of platelets, causing a decrease in their numbers. While the exact mechanism is not fully understood, it is believed that omeprazole may trigger an immune response that targets platelets, leading to their destruction.
Factors to Consider
It is important to note that not everyone who takes omeprazole will develop thrombocytopenia. The risk of this side effect is relatively rare, but individuals with a history of blood disorders or hypersensitivity reactions may be at a higher risk.
If you are taking omeprazole and experience symptoms such as easy bruising, bleeding gums, or frequent nosebleeds, it is important to consult your healthcare provider. They can perform blood tests to determine your platelet levels and assess whether omeprazole may be a contributing factor.
Role of Omeprazole in Thrombocytopenia
Omeprazole is a medication commonly used to treat conditions such as acid reflux, ulcers, and other gastrointestinal issues. While omeprazole is generally well-tolerated by most individuals, there have been reports of thrombocytopenia occurring as a rare side effect of this medication.
Thrombocytopenia is a condition characterized by a low platelet count in the blood. Platelets are important for blood clotting, and low levels of platelets can lead to increased risk of bleeding and bruising.
How does Omeprazole cause Thrombocytopenia?
The exact mechanism by which omeprazole may cause thrombocytopenia is not fully understood. It is believed that omeprazole may affect the production or survival of platelets in the bone marrow, leading to decreased platelet count.
If you are taking omeprazole and experience symptoms such as easy bruising, nosebleeds, or prolonged bleeding, it is important to consult your healthcare provider for further evaluation and management.
Symptoms
Thrombocytopenia is a condition characterized by a low platelet count in the blood. The symptoms of thrombocytopenia can vary depending on the severity of the condition. Common symptoms of thrombocytopenia may include:
Mild Thrombocytopenia
– Easy bruising
– Prolonged bleeding from minor cuts or injuries
– Petechiae (small red or purple spots on the skin)
Severe Thrombocytopenia
– Excessive bleeding from minor cuts or injuries
– Heavy menstrual periods in women
– Bleeding gums
– Blood in the urine or stool
If you experience any of these symptoms, it is important to consult a healthcare provider for further evaluation and management of thrombocytopenia.
| Severity | Symptoms |
|---|---|
| Mild Thrombocytopenia | Easy bruising, Prolonged bleeding, Petechiae |
| Severe Thrombocytopenia | Excessive bleeding, Heavy menstrual periods, Bleeding gums, Blood in urine/stool |
Recognizing Thrombocytopenia
Thrombocytopenia can be recognized through a combination of symptoms and diagnostic tests. Some common signs of thrombocytopenia include easy bruising, prolonged bleeding from minor cuts or injuries, frequent nosebleeds, blood in the urine or stool, and petechiae (small red or purple spots on the skin).
Additionally, thrombocytopenia can be diagnosed through a blood test called a complete blood count (CBC), which measures the number of platelets in the blood. A low platelet count (thrombocytopenia) is typically defined as a platelet count below 150,000 platelets per microliter of blood.
Key Points to Remember:
- Pay attention to unusual bruising or bleeding that does not seem to be triggered by an injury.
- Seek medical attention if you experience frequent nosebleeds or unexplained bruising.
- A CBC test can confirm the presence of thrombocytopenia by measuring platelet levels in the blood.
| Recognizing Thrombocytopenia | Diagnosis |
|---|---|
| Easy bruising | Blood test – CBC |
| Prolonged bleeding | Platelet count below 150,000 |
| Nosebleeds |
Diagnosis
Diagnosing thrombocytopenia involves a series of tests and examinations to determine the cause of low platelet count. The first step in the diagnosis is a physical examination and medical history review to identify any underlying conditions that may contribute to the development of thrombocytopenia. The healthcare provider may ask about symptoms, medications, and family history.
After the initial assessment, diagnostic tests will be ordered to confirm the diagnosis. Blood tests, including a complete blood count (CBC) with differential, will be performed to measure the platelet count and examine the other blood components. Additional tests, such as a peripheral blood smear, bone marrow aspiration, and immunological tests, may also be recommended to identify the specific cause of thrombocytopenia.
Once the diagnosis is confirmed, the healthcare provider will work with the patient to develop a treatment plan tailored to the underlying cause of thrombocytopenia. Close monitoring and follow-up may be necessary to track the platelet count and adjust treatment as needed.
Testing for Thrombocytopenia
Diagnosing thrombocytopenia involves conducting various tests to determine the platelet count in the blood. Below are some common tests used to detect thrombocytopenia:
- Complete Blood Count (CBC): This test measures the number of platelets, red blood cells, and white blood cells in the blood. A low platelet count may indicate thrombocytopenia.
- Peripheral Blood Smear: A blood smear is examined under a microscope to assess the size, shape, and number of platelets. Abnormalities in platelet morphology can suggest thrombocytopenia.
- Bone Marrow Aspiration: In some cases, a sample of bone marrow is taken and examined to determine the production of platelets. This test helps identify the underlying cause of thrombocytopenia.
- Platelet Function Tests: These tests assess the function of platelets in clot formation. Abnormal platelet function can contribute to thrombocytopenia.
It is essential to consult a healthcare provider for proper evaluation and diagnosis of thrombocytopenia. Treatment options can vary depending on the underlying cause and severity of the condition.
